AARP Hearing Center


You already know it’s important to get your flu vaccine every year, ideally by the end of October. And when you go in for the shot, it’s a great time to make sure you’re up-to-date on all the other immunizations you should be receiving as an adult.
After all, it’s not just babies and youngsters who need a poke to protect against serious, and potentially lethal, diseases. Adults need them too, especially as our immune systems weaken with age.
So what shots should you get at 50 and beyond?
“There are new vaccines that have come out in the past several years, specifically aimed at older adults,” says Morgan Katz, M.D., an assistant professor of medicine at Johns Hopkins University School of Medicine. Take for example, the new RSV vaccine, which was approved last year.
Another is Shingrix, the amazingly effective shingles vaccine. And a few pneumococcal vaccines are on the market as well.
Below you’ll find the vaccinations every adult needs, followed by two — for hepatitis A and B — that you need only if you have certain risk factors.
What you won’t see on the list? Measles and chicken pox vaccines. Anyone born before 1957 doesn’t need a measles vaccine because the disease was so prevalent when they grew up that immunity as an adult is assumed, though the Centers for Disease Control and Prevention (CDC) says adults who do not have presumed immunity should get at least one dose of MMR (measles-mumps-rubella) vaccine.
Chicken pox is similar in that most adults already have immunity from childhood exposure to the disease, Katz says.
“Almost all adults over 40 have been exposed to chicken pox,” she says, noting that it would be “an extremely rare case” for an adult not to have been. That said, if you think you could be in that tiny minority, ask your doctor about getting the chicken pox vaccine as an adult.
For the rest of the list, you can get your necessary shots at doctors’ offices, pharmacies, workplaces, community health clinics and other locations. And most health insurance plans will pick up the tab. So stop in and let ’em stick it to you.
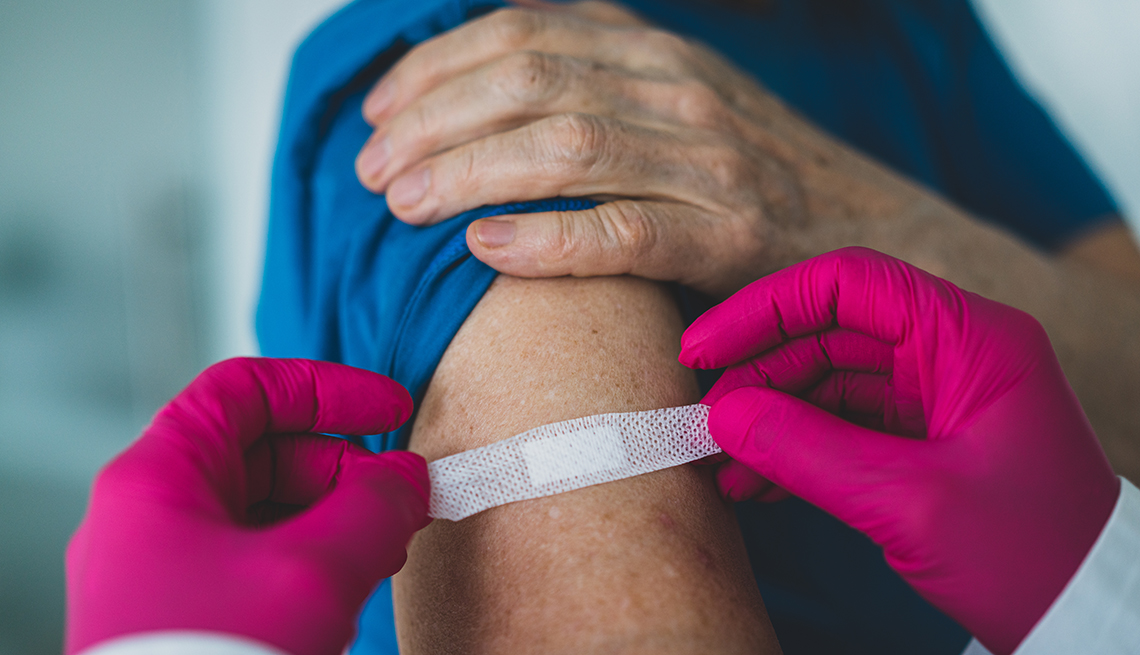
1. Influenza vaccine
Who needs it: All adults, no matter the age.
How often: Once a year. “The virus itself changes every year,” Katz says. “Researchers try to predict what will be the most common strain that season, then reformulate the vaccine accordingly.” Flu season typically begins in October and ends in March, so the CDC recommends rolling up your sleeve by the end of October, since it takes about two weeks after a vaccination for flu-fighting antibodies to develop in the body.
What you need: Adults 65 and older should make sure they receive a high-dose version of the shot. The options include:
- Fluzone High-Dose Quadrivalent is an injectable vaccine that contains four times the antigen (the flu proteins that our immune system recognizes and attacks) of a standard-dose inactivated flu vaccine, to help create a stronger immune response.
- Fluad Quadrivalent is an adjuvanted flu vaccine, made with an MF59 adjuvant, an additive that creates a more robust immune response.
- Flublok Quadrivalent. This is a recombinant vaccine, which means it does not require an egg-grown virus and does not use chicken eggs in the manufacturing process. This may be a good option if you are allergic to eggs (the Fluzone and Fluad offerings are grown in eggs). Flublok Quadrivalent contains three times the antigen of other standard-dose inactivated flu vaccines.
Why you need it: Each year, the flu is to blame for hundreds of thousands of hospitalizations and tens of thousands of deaths, and older adults are at higher risk for these serious outcomes. Fifty to 70 percent of flu-related hospitalizations occur among people 65 and older, according to the CDC, and 70 to 85 percent of flu-related deaths occur among this age group.
Talk to your doctor if: You’ve had a severe reaction to the flu shot in the past, are allergic to eggs, have (or have had) Guillain-Barré syndrome or have a fever. (In that case, you’ll likely be asked to wait until your temp is back to normal before you get the vaccine.)
Parting shot: Even if you’re vaccinated, there’s a possibility you could get the flu. How well the inoculation protects depends on different factors, including your age and health status. That said, a flu vaccination may lessen the severity of illness if you do get sick. Research, including a study published Aug. 29, 2024, finds that flu vaccination reduces flu-related hospitalizations and deaths, including among older adults.





































































More on Health
Older Adults Still Feel Effects of COVID-19 Pandemic
Though much has changed since the early days of the COVID-19 pandemic, the toll is still felt — overwhelmingly by older Americans.How to Choose a Top-Notch Doctor as You Age
Physician Sharon Malone, author of ‘Grown Woman Talk,’ tells us what to consider when looking for the best care
Have COVID-19? Here’s How Long You Need to Isolate
CDC updates guidelines for people with a coronavirus infectionRecommended for You